Haematinics
- 1. Amity Institute of Pharmacy 1 AMITY UNIVERSITY UTTAR PRADESH AMITY INSTITUTE OF PHARMACY LUCKNOW 2018-20Presented by- Afreen Hashmi M.Pharm.(Pharmacology) 1st sem Enroll no. A8454918005 Guided by- Dr. Himani Awasthi Associate Professor Department of Pharmacology Amity Institute of Pharmacy Heamatinics
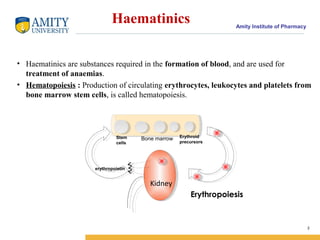
- 2. Amity Institute of Pharmacy Haematinics • Haematinics are substances required in the formation of blood, and are used for treatment of anaemias. • Hematopoiesis : Production of circulating erythrocytes, leukocytes and platelets from bone marrow stem cells, is called hematopoiesis. 2 Kidney Bone marrow erythropoietin Erythroid precursors Stem cells Erythropoiesis
- 3. Amity Institute of Pharmacy Anaemia is reduced concentration of haemoglobin in the blood i.e. deficiency in oxygen-carrying erythrocytes. Normal values: Male = 13.2 -17.0 g/dL Normal values: Female = 12.0 -16.0 g/dL Causes : • Anaemia occurs when balance between production and destruction of RBCs are disturbed by : i) Blood loss (acute or chronic) for eg. In menstruation and trauma conditions. ii) Increased destruction of RBCs ( i. e. hemolytic anemia) iii) Impaired red cell formation due to – Deficiency of iron, Vitamin B12, folic acid. – Bone marrow depression caused by : 3 Anaemia
- 4. Amity Institute of Pharmacy drug toxicity (e.g. anticancer drug) radiation therapy disease of bone marrow reduce production of erythropoietin (e.g. chronic renal failure, RA, AIDS) Types of Anaemia 1.Microcytic Anaemia : deficiency of Iron. 2.Macrocytic Anaemia : deficiency of folic acid and B12. 3.Pernicious Anaemia : Lack of intrinsic factor INF. 4.Aplastic Anaemia : due to Bone marrow dysfunction. 5.Haemolytic anaemia : Excessive haemolysis. 6.Sickle cell anaemia : Sickle shaped RBCs. 4
- 5. Amity Institute of PharmacySymptoms of Anaemia The main symptom of anaemia is fatigue but, especially if it is chronic, is often surprisingly asymptomatic. Other symptoms include : •weakness, •pale skin, •rapid heartbeat, •shortness of breath. •chest pain, •dizziness, •irritability (in children with anaemia), •coldness in hands and feet. 5
- 6. Amity Institute of Pharmacy Classification of Haematinics A. IRON 1. Oral preparations of iron (Fe2+ ) Ferrous sulfate Ferrous succinate Ferrous aminoate Ferrous fumarate Ferrous gluconate Carbonyl iron B. Maturation factor : Vitamin B12 : Cyanocobalamin, Hydroxocobalamin, Methylcobalamin. Folic acid : Folinic acid (Leucovorin, Fastovorin ). C. Hematopoietic Growth Factors : Erythropoietin: Epoetin alfa, Epoetin beta, Darbepoetin alfa 6 2. Parenteral preparations of iron (Fe3+ ) Iron dextran Iron-sorbitol-citric acid Iron sucrose Ferric carboxymaltose
- 7. Amity Institute of Pharmacy IRON • All body cells need iron. It is crucial for oxygen transport, energy production, and cellular growth and proliferation. • The human body contains an average 3.5 g of iron (males 4 g, females 3 g). • Typical daily normal diet contains 10–20 mg of iron. 5 - 10% of ingested iron is absorbed i.e. 1-2mg. • Daily loss is about – 0.5-1mg. Distribution : • About 65% iron circulates in blood as haemoglobin. • 25% stored in Liver, spleen and bone marrow as Ferritin and haemosiderin available for haemoglobin synthesis. • Rest present in Myoglobin, cytochrome and various enzymes. 7
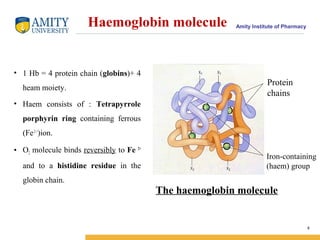
- 8. Amity Institute of PharmacyHaemoglobin molecule • 1 Hb = 4 protein chain (globins)+ 4 heam moiety. • Haem consists of : Tetrapyrrole porphyrin ring containing ferrous (Fe2 + )ion. • O2 molecule binds reversibly to Fe 2+ and to a histidine residue in the globin chain. 8 Protein chains Iron-containing (haem) group The haemoglobin molecule
- 9. Amity Institute of PharmacyIron : Absorption • Site of absorption - duodenum and upper jejunum. • In stomach iron dissolves and binds to mucoprotein (carrier). Dietary iron in ferric form (Fe3 + ) is low soluble in neutral pH and not absorb. Reduce to ferrous form (Fe2 + ) + vitamin C. Soluble iron-ascorbate chelate Absorption occurs. 9 Ascorbic acid
- 10. Amity Institute of PharmacyIron : transport Iron enters in plasma in ferrous form oxidise Immediately into ferric form Complex with transferrin a carrier (glycoprotein) 10 Storage in the mucosal cell as ferritin To the plasma
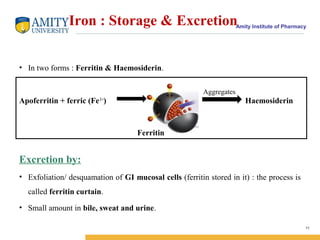
- 11. Amity Institute of Pharmacy Iron : Storage & Excretion • In two forms : Ferritin & Haemosiderin. Apoferritin + ferric (Fe3 + ) Haemosiderin Excretion by: • Exfoliation/ desquamation of GI mucosal cells (ferritin stored in it) : the process is called ferritin curtain. • Small amount in bile, sweat and urine. 11 Aggregates Ferritin
- 12. Amity Institute of Pharmacy Iron Preparations Oral Iron Preparations : •Preferred route. •Dissociable ferrous salts : inexpensive, increased iron content, better absorbed. – Ferrous Sulfate - Cheapest form of Iron and one of the most widely used. – Side Effects are extremely mild: • Nausea, upper abdominal pain, constipation or diarrhea. Parenteral Iron Preparations May be given when- •Oral iron not tolerated : bowel upset is too much. •Not absorbed orally : malabsorption, surgical procedures, inflammatory condition (RA). •In patients with : chronic renal failure, chemotherapy-induced anaemia. 12
- 13. Amity Institute of Pharmacy Parenteral Iron Preparations • Iron-dextran: slow iv or deep im (50mg/ml) circulated without binding to transferrin, not excreted in urine or in bile. • Iron-sorbitol-citric acid: only im (not favored now because producing higher side effects. • Iron sucrose : iv injection Less side effects, safer drug than older preparations. • Ferric carboxymaltose : iv only less side effects, anaphylaxis is rare. 13
- 14. Amity Institute of Pharmacy Toxicity of Iron Overload • Acute iron toxicity • Chronic iron toxicity • Treated by : Desferrioxamine – an iron chelator (DOC) - It bound with ferric & unbound iron, not absorbed from the gut & prevent its absorption. - In severe poisoning, it is given by slow iv infusion. Deferiprone - orally absorbed iron chelator 14
- 15. Amity Institute of Pharmacy Clinical Uses of Iron • To treat iron deficiency anaemia which can be caused by: -chronic blood loss (e.g. menorrhagia, trauma, colon cancer) -increased demand (e.g. in pregnancy and premature babies, menstruating womens) -Inadequate dietary intake -Inadequate absorption (e.g. following gastrectomy) • In GI Bleeding due to: Ulcers, Aspirin, Excess consumption of coffee 15
- 16. Amity Institute of Pharmacy Maturation factors : Vitamin B12 • A B12 deficiency will cause a pernicious anemia and it take up to two years to develop. • Source: In food, especially in liver and kidneys. • Vitamin B12 is essential for cell growth and multiplication • Absorption of B12 : binds with intrinsic factor (IF) in the stomach. The B12-IF complex then travels through the small intestine and is absorbed in the distal ileum. 16 Distal ileum Site of B12 absorption Oesophagus Stomach IF Intrinsic factor Vitamin B12 ingested
- 17. Amity Institute of Pharmacy Maturation factors : Vitamin B12 • Cyanocobalamine • Hydroxycobalamine • Methylcobalamine Actions • Vitamin B12 is required for two main reactions : – The conversion of methyl-FH4(inactive) to FH4(active). Necessary for normal DNA synthesis. – The conversion of methylmalonyl-CoA to succinyl-CoA. 17
- 18. Amity Institute of Pharmacy Maturation factors : Folic acid • Source in food – yeast, egg yolk, liver and leafy vegetables. • Folic Acid is absorbed in the small intestines. • Folic Acid deficiency (F.A. Deficiency) is also called Will’s Disease. • Deficiency may produce megaloblastic anemia; teratogenic effects. • Folic acid and vitamin B12 required for maturation of haemoglobin. Actions of Folic acid • Folic acid is inactive and is converted to tetrahydrofolate by dihydrofolate reductase. • This enzyme reduces dietary folic acid to FH4 and also regenerates FH4 from FH2. • It is generally given orally. • Folinic acid is synthetic preparation of folic acid. 18
- 19. Amity Institute of PharmacyUses of Folic acid 1) In megaloblastic anaemia due to inadequate dietary intake of folic acid • Can be due to chronic alcoholism, malabsorption syndromes, cancer or hepatic disease. 1) Increased demand : pregnancy, lactation, premature infancy, RA, etc. 19
- 20. Amity Institute of Pharmacy Haemopoietic Growth Factors • Erythropoietin is required for erythropoiesis. • Erythropoietin is a hormone produced in juxtatubular cells in the kidney which regulated division and differentiation of blood cells. • Erythropoietin deficiency also results in anaemia. • Erythropoietin preparations : 1.Epoeitin α and β (recombinant erythropoietin) ; given parenteraly only. 2.Darbopoeitin ; is longer acting preparation. 20
- 21. Amity Institute of Pharmacy Clinical Uses of Epoietin Anaemia due to: • Chronic renal failure. • Cancer chemotherapy. • AIDS. • Premature infants. • Chronic inflammatory disorders (RA). • In Chronic Heamolytic Anaemia. 21
- 22. Amity Institute of Pharmacy Refrence • Rang & Dale’s Pharmacology 6th Edition • Bertram G.Katzung Basic And Clinical Pharmacology • Principles Of Pharmacology Hl.Sharma Kk.Sharma • http://slideshare.com • http://slideplayer.com 22